- Dragon Speech Recognition Software
Don’t waste time typing. Getting trained in the expedience of Dragon software will have you updating EHR measures in no time. This allows you more time to provide quality care to your patients. Schedule a DEMO to see how effectively Dragon works in all applications. - Helpful Acronym Definitions
MACRA – Medicare Access and CHIP Reauthorization Act
HHS – Health and Human Services
QPP – Quality Payment Program
MIPS – Merit-Based Incentive Payment System (Replaces the Sustainable Growth Rate (SGR) formula)
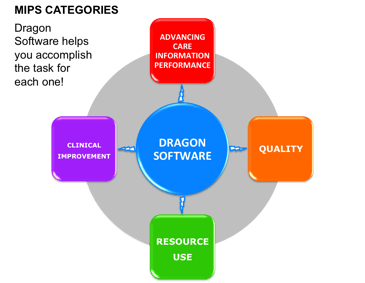
- Quality – Replaces Physician Quality Reporting System (PQRS) Requires reporting on six quality measures, or one specific or subspecialty specific measure set.
- Clinical Improvement Activities – New Category - Four medium weighted or two high-weighted activities to receive full credit.
- Advancing Care Information – Replaces Meaningful Use (MU) Using Certified Electronic Health Record Technology (CEHRT) report on five required measures.
- Cost – Replaces the Value-Based Modifier (Will be calculated in 2017, but will not determine payment adjustment until 2018.)
-
APM – Alternative Payment Model
AAPM– Advanced Alternative Payment Mode
EC – Eligible Clinician
ACI – Advancing Care Information
-
All of these can be more clearly defined at:http://www.aafp.org/practice-management/payment/medicare-payment/acronyms.html
- Website Help
There are resources to help define what you need:
https://qpp.cms.gov
https://www.healthcatalyst.com/wp-content/uploads/2017/01/Preparing-for-MACRA.pdfhttps://www.gpo.gov/fdsys/pkg/FR-2016-11-04/pdf/2016-25240.pdf
Although it is too late to start reporting for 2017 (the deadline was October 2nd.) It is not too late to start preparing for 2018. The consequences of ignoring QPP reporting are a 4% reduction to Medicare reimbursement (starting 2019) and more importantly, reputations are at stake, as quality scores will be made public.
Know the intent of MACRA is not just to save money but also to take care of patients efficiently and give them the best quality care. It is about value over volume.


